Separately, several states, including California, Connecticut, Florida, Georgia, Illinois, Indiana, Maine, Maryland, New Hampshire, New Jersey , New York and Virginia issued even more stringent screening and quarantine orders to prevent the spread of Ebola within their borders, according to a legal analysis by Arizona State University law professor James Hodge for the Network for Public Health Law.
The primary source of money for such efforts, the CDC's Public Health Emergency Preparedness cooperative agreement, began after the 2001 terrorist attacks in New York and Washington, D.C. to better prepare the nation’s public health system in emergency situations. But since then, funding has dipped from a high of more than $1 billion in 2006 to $585 million last year.
Another funding stream, the federal Hospital Preparedness Program administered by the US Department of Health and Human Services, was launched around the same time to prepare health care workers for terrorist attacks, natural disasters, widespread foodborne illnesses and infectious disease outbreaks. But funding has fallen from $515 million in 2004 to $255 million this year.
In addition, many states have made cuts to their own public health preparedness funding. Depending on where you live, federal funding for state and local public health preparedness comprises 75 to 90 percent of the total budget, with the rest made up of state and local funds.
Varying States of Readiness
"There is no uniformity among public health systems across the country," said Jack Hermann, chief program officer of the National Association of City and County Health Officials.
Smaller jurisdictions may be more challenged because they have fewer resources, but they may have the advantage of everyone knowing everyone else. “Sometimes, the fire chief and the top health official are the same person,” Hermann said.
Public health's most important resource is people — trained health care workers, analysts and educators, Blumenstock said. Even if Congress does appropriate more money in response to the current Ebola situation, finding and training those people won’t happen overnight.
State and local public health agencies learned the hard way that they needed to develop 'administrative preparedness' by streamlining the hiring and contracting process, he said. During the H1N1 (swine flu) pandemic in 2009-2010, Congress appropriated $1.5 billion to help state and local governments fight its spread. "It took too long to convert those emergency funds into services in the community," Blumenstock said. "We're all optimistic we’ll do a better job of that this time."
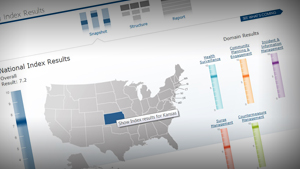
Last year, the CDC and other federal agencies, state health officials, nonprofits and research groups for the first time released a broad index of state public health readiness that goes beyond health agencies to include first responders, schools, volunteer organizations and other state agencies and community groups. The rating system, known as the National Health Security Preparedness Index, uses a variety of sources, such as CDC audit results and hospital data, to rate each state's readiness on a scale of one to 10, with 10 being the best. The national average in 2013 was 7.2.
Massachusetts was the most prepared, followed by Rhode Island, Virginia, North Dakota, New York, Maryland, Connecticut and Vermont. Least prepared for a public health emergency was Nevada, followed by Alaska, Louisiana, Idaho, Montana, Arkansas, Georgia, Kansas and Mississippi.
Part of the measurement is based on performance in real-life situations, such as preparing for a possible Ebola outbreak. This year’s report is scheduled for release later this month.
Airports of Entry
So far, the states hardest hit by the Ebola response effort have been those with airports designated by the CDC for screening of incoming passengers from West Africa: Georgia, Illinois, Maryland, New Jersey, New York and Virginia. "We're not in a panic now, but we're starting to get tired," said David Trump, deputy commissioner for public health and preparedness in Virginia’s health department.
Trump said employees in his agency have been working overtime since August, and many have been reassigned. Some with administrative and other routine jobs are now on the front lines, contacting and monitoring people who have flown into Dulles International Airport from West African countries.
As many as 50 passengers arrive in Dulles each day from Liberia, Sierra Leone or Guinea. Most are returning US residents and most are boarding connecting flights to a final destination outside of Virginia. As of last week, public health workers were monitoring 81 Virginia residents who had traveled from West Africa. That number is likely to rise in the next couple of months to between 200 and 300 and remain at that level for the foreseeable future, Trump said.
More Articles
- Monetary Policy Report Prepared at the Federal Reserve Bank of Richmond, Expectations for Future Growth Were Mostly Unchanged
- Ferida Wolff Writes: This Holiday Season
- Journalist's Resource: Religious Exemptions and Required Vaccines; Examining the Research
- Consumer Financial Protection Bureau (CFPB): Lenders Cannot Discriminate Based on Sexual Orientation or Gender Identity
- Kaiser Family Foundation (KFF), February 8th: This Early Stage of the COVID-19 Vaccine Roll-Out, Most Older Adults Have Not Yet Been Vaccinated As Supply Remains Limited
- The GAO Finds: Elder Financial Exploitation — The Fraudulent or IIlegal Use of An Older Adult's Funds or Property — Has Far-reaching Effects on Victims and Society
- Pew Trusts, Stateline: Poverty Grows Despite Economic Recovery; Left Behind
- How are States Prioritizing Who Will Get the COVID-19 Vaccine First? CDC’s Advisory Committee on Immunization Practices (ACIP) Released an Interim Recommendation For the Highest Priority Group
- Stateline: Many Faithful Say It’s Time to Gather. Some Governors Disagree
- Pew Trust's Stateline: Staffing Nursing Homes Was Hard Before the Pandemic. Now It’s Even Tougher.