Notes: *Other sources refer to insurance provided by a single source or multiple sources, excluding Medicare (e.g. Medicaid only, Tricare only). ** Medicare only refers to beneficiaries with Part A or Parts A and B only. *** Due to self-reporting biases, the percentage of older adults covered by Medicare Advantage plans is likely to exclude beneficiaries who have employer sponsored coverage or Medicaid coverage through Medicare Advantage plans. **** Employer sponsored includes retiree coverage and coverage for older adults currently employed.
The persistence of unpaid medical bills among older adults with more comprehensive insurance coverage is at least in part the result of inaccurate bills.32 Studies have found that erroneous insurance claims commonly result in inaccurate bills for patients with insurance.33 Common errors—such as missing or invalid claim data, authorization and pre-certification issues, missing medical documentation, incorrect billing codes, and untimely filing—contribute to the rejection of claims that would otherwise be paid.34 Many of these errors likely are avoidable or fixable,35 but only a fraction of rejected claims are adjusted and resubmitted.36 A 2022 survey found that 68 percent of adults with unpaid medical bills in the past five years reported that they did not pay the medical bill in full or only partially paid it because they thought their insurance was covering it. According to the survey, 44 percent of adults reported that they did not pay the medical bill in full or only partially paid it because they were not sure if the medical bill was accurate.37
Older adults face a complex billing system with a high likelihood of errors and inaccurate bills
While inaccurate medical billing and the burden of addressing inaccurate bills affect consumers of all ages, two factors increase the chances of errors and inaccurate bills for older adults.
First, older adults are more likely than younger adults to have multiple chronic health conditions38 that require complex medical care.39 Providers use “higher-intensity” medical billing codes to seek reimbursement for higher-level care.40 These billing codes provide for larger payments, but they also require detailed documentation.41 Medical claims using these codes are facing greater scrutiny from insurers due to concerns about upcoding42 and overuse.43 These factors are commonly associated with billing errors and claim denials.
Second, older adults are also more likely to rely on multiple insurance plans to cover their medical services, compared to adults ages 18 to 64. In 2020, 68 percent of older adults with unpaid medical bills were covered by two or more sources of insurance, compared to 11 percent of adults ages 18 to 64 with unpaid medical bills.44 Studies have found that having multiple insurers increases the complexity of the billing process.45
In cases involving multiple payers, Medicare relies on coordination agreements that allow claims to be shared and transmitted to multiple insurers simultaneously.46 The transmission of claims between Medicare and other insurers is known as the crossover process.47 The submission of accurate claims is particularly important because the crossover process does not necessarily fix breakdowns in communication between insurers and providers, or resolve data conflicts.48 To further complicate the billing system, some insurers, including state Medicaid agencies, require certain claims to be filed directly with them instead of relying on the crossover process.49 When providers fail to file directly with these insurers, this inaction results in unpaid bills.
Lastly, when multiple insurers are involved, each insurer sets a different reimbursement rate or discount. This limits the amounts that providers receive from insurers and/or can collect from beneficiaries.50 Yet some providers wrongfully demand payment for the difference between their bill and the contractual reimbursement rate or discount, in addition to allowable coinsurance, copayments, and deductibles.51
CFPB debt collection complaints involving Medicare show that inaccurate billing is a common issue, especially for consumers who rely on more than one insurance source. In 53 percent of these complaints, people with Medicare reported that the underlying debt was inaccurate. For people with more than one source of insurance, the proportion was 61 percent.52
FIGURE 3
Issues reported in medical debt collection complaints related to Medicare, January 2020 – December 2022
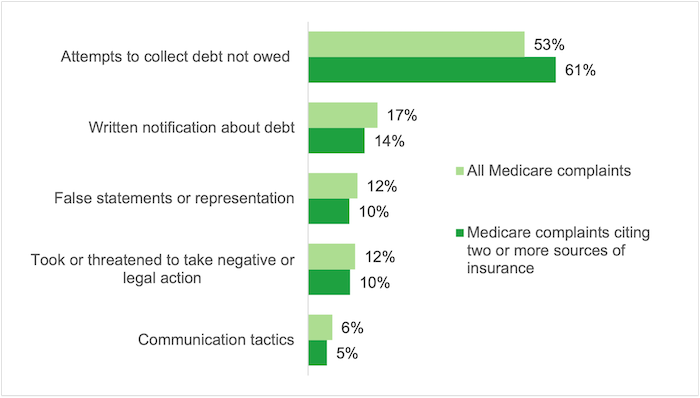
Source: CFPB Consumer Complaints
The complaints describe in detail issues that lead to inaccurate and erroneous billing for people with multiple sources of insurance. For example, some complaints report that providers never billed a secondary insurer such as Medicaid or Tricare.
More Articles
- Medicare Advantage Increasingly Popular With Seniors — But Not Hospitals and Doctors
- Julia Sneden Redux: Age Rage; Sometimes You Just Have to Strike Back
- Kaiser Health News*: May 11th Era of ‘Free’ Covid Vaccines, Test Kits, and Treatments Is Ending. Who Will Pay the Tab Now?
- Congressional Budget Office: Federal Budget Deficit Totals $1.4 Trillion in 2023; Annual Deficits Average $2.0 Trillion Over the 2024–2033 Period
- Shhhhhh by Ferida Wolff
- Women Consistently Earn Less Than Men; Women Are Over-represented in Lower Paying Jobs and, As They Age, the Pay Gap Widens Even More
- Rose Madeline Mula Writes: I’ve Got A Secret – NOT!
- Government of Canada Renews Investment in Largest Canadian Study on Aging
- Rose Madeline Mula Writes: I Feel Like That Carton of Milk In the Refrigerator Which Is Beyond Its Expiration Date
- Julia Sneden Writes: Age Rage; Sometimes You Just Have to Strike Back






